Osteopenia and Osteoporosis The Difference Between The Two
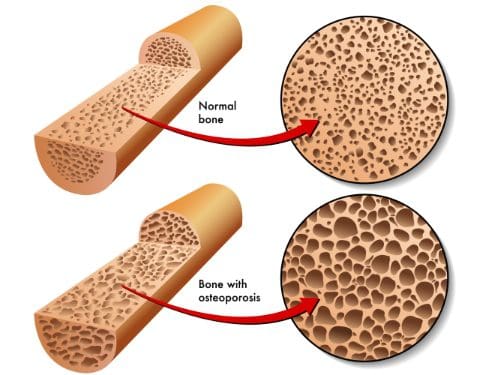
Osteopenia and osteoporosis are very similar. Both conditions are defined as decreased bone density, but osteopenia is the less severe of the two. Osteopenia can still pose a problem because it can increase a person’s chances of breaking a bone.
What are the symptoms?
Osteopenia usually doesn’t cause symptoms unless a bone is broken. However, some patients who present with osteopenia complain of dull back pain.
Symptoms associated with osteoporosis include the following:
- Back pain, caused by a fractured or collapsed vertebra
- Loss of height over time
- A stooped posture
- A bone fracture that occurs much more easily than expected
What are the causes and who is at risk?
Women (primarily small-boned Caucasian and Asian) are most at risk for both conditions, primarily those who are age 65 or older as well as women who are postmenopausal. However, men can also be affected.
Anyone who meets any of the criteria for being at risk for either of the bone conditions should be evaluated. Often, catching the conditions early can make a significant difference in the effects that they have on the body and in some cases, can even be arrested so that they don’t progress.
Some of the common causes of both conditions include:
- Lifestyle habits
- Smoking
- Insufficient calcium
- Sedentary lifestyle
- Excessive alcohol consumption
- Vitamin D deficiency
- Carbonated beverages
- Medical Situations
- Bulimia, anorexia, and other eating disorders
- Estrogen deficiency in women
- Certain hormone imbalances
- Overactive thyroid
- Certain treatments including radiation and chemotherapy
- Low testosterone in men
- Medications including anti-seizure, hydrocortisone, and steroids
- Health issues
- Tumors
- Cystic fibrosis
- Crohn’s disease
- Digestive issues
It should also be noted that certain types of diets, particularly those that advocate extremely low fat, or no fat can also cause problems. Vitamin D is necessary for calcium absorption in the body, but vitamin D is a fat-soluble vitamin meaning the body requires some fat in order to make use of it. When there is inadequate fat, the vitamin cannot be absorbed and in turn, calcium cannot be absorbed.
A family history of osteopenia, osteoporosis, or low bone mass can increase a person risk by 50% to 85%.
How is it diagnosed?
Bone mineral density (BMD) tests are used to diagnose both osteopenia and osteoporosis by measuring the calcium levels in bone. This type of test can also provide an estimate of how much at risk a person is for bone fractures.
This test is painless and non-invasive. It is usually performed on the heel, shin bone, wrist, spine, finger, or hip.
Two common types of these tests are radiographs, a standard diagnostic tool for osteopenia, and Dual Energy X-ray Absorptiometry (DEXA). A DEXA scan is essentially a low energy x-ray so patients are not exposed to as much radiation as they would be if they had a regular x-ray. The results are attained by comparing the score (measurements were taken) to scans of individuals who do not have the condition.
Once the score is measured and compared, it is assessed using a chart that identifies the level or risk:
- +1.0 to -1.0Â -Â Normal bone density
- -1.0 to -2.5Â -Â Low bone density
- -2.5 or higher - At risk for osteoporosis
What are the treatments?

As with most conditions, prevention is the most effective treatment. If you have a family history or fall under any of the risk factors, there are things you can do to minimize the effects or prevent the conditions completely.
Your chiropractor can talk to you about lifestyle changes, exercise, and diet as well as supplements that you can take. Chiropractic adjustments can also be effective for many patients with osteopenia and osteoporosis as long as the chosen technique is a low force technique like Activator.
Many patients find these natural treatments preferable to any medications that may be prescribed. The most important thing you should do, though, is to get a bone density test if you are in an at-risk category, is a woman who is postmenopausal or age 65 or older.
El Paso, TX Chiropractor Shoulder Pain Treatment
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Osteopenia and Osteoporosis The Difference Between The Two" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933








Comments are closed.