Spondylolisthesis occurs when a vertebra of the spine slips forward over the vertebra below it. Spondylolisthesis can be categorized as: congenital spondylolisthesis, which means the disorder is present at birth; isthmic spondylolisthesis, which occurs when a defect occurs in a supportive vertebral structure of the spine; and degenerative spondylolisthesis, which is more common and is frequently associated with degenerative disc disease, or DDD, where the intervertebral discs lose hydration with age.
Development of Spondylolisthesis
The spinal column is exposed to directional pressures while it carries, absorbs, and also distributes most of the fat of the body throughout physical activities and during rest. To put it differently, while the spine is consuming and carrying body fat, additionally, it moves in different directions (e.g., rotate, bend forwards ). This mixture of functions causes unnecessary stress to be placed onto the vertebra and the supportive vertebral structures of the spine, and it might result in one of these slipping forwards over the ones beneath it, ultimately developing into spondylolisthesis.
Grading spondylolisthesis
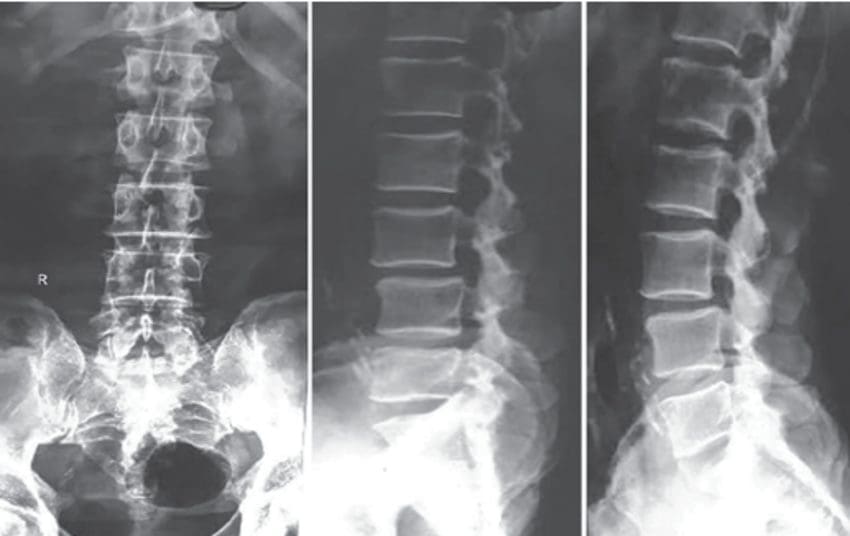
Doctors “grade” the severity of spondylolisthesis utilizing five descriptive categories. Even though there are several factors your physician notes when evaluating your spondylolisthesis, the grading scale (below) relies on how far forward a vertebral body has slid over the vertebra beneath it. Often, the doctor uses a lateral (side view) x-ray to examine and grade spondylolisthesis. Grade I is a smaller slide than Grade IV or V.
- Grade I: Less than 25% slip
- Grade II: 25% to 49% slip.
- Grade III: 50% to 74% slip.
- Grade IV: 75% to 99% slip.
- Grade V: The vertebra has fallen forward off the vertebra below it. This grade is the most severe type of spondylolisthesis and is medically referred to as spondyloptosis.
Who Might be at Risk
If a family member has spondylolisthesis, your risk for developing the disorder may be higher. Also, some physical activities can make you more vulnerable to developing spondylolisthesis. Gymnasts, linemen in football, and weightlifters, all put pressure and stress on their spine. Additionally, being involved in an automobile accident or other personal injury circumstance can lead to spinal injury, in this instance, such which may cause spondylolisthesis. Those motions can place
Curated by Dr. Alex Jimenez

Additional Topics: Scoliosis Pain and Chiropractic
The spine is a complex structure made up of bones, joints, ligaments, and muscles, among other soft tissues. Because of this, injuries and/or aggravated conditions, such as herniated discs, can eventually lead to symptoms of back pain. Sports injuries or automobile accident injuries are often the most frequent cause of back pain, however, other aggravated conditions can also cause back pain. Scoliosis is a well-known, health issue characterized by an abnormal curvature of the spine and it is subcategorized by cause as a secondary condition, idiopathic, or of unknown cause, or congenital. Fortunately, alternative treatment options, such as chiropractic care, can help ease back pain associated with scoliosis through the use of spinal adjustments and manual manipulations, ultimately improving pain relief. Chiropractic care can help restore the normal curvature of the spine.

EXTRA EXTRA | IMPORTANT TOPIC: Chiropractic Massage Therapy
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Classifying Spondylolisthesis After a Personal Injury" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933







Comments are closed.