Spinal Stimulation and Chronic Back Pain
Spinal stimulation is a treatment option that could help relieve pain and improve the quality of life for individuals dealing with chronic pain, like low back and leg pain. Spinal stimulation can help reduce and manage chronic pain that does not alleviate or reduce with physical therapy, pain medications, injections, and other non-surgical treatments/therapies. Â
A spinal stimulator is a tiny device that is implanted underneath the skin. It is a form of neuromodulation that works by blocking pain signals the nerves send out from reaching the brain. The device delivers a very low electrical impulse that masks/changes pain signals before reaching the brain.
Â
A Spinal Stimulation System
Â
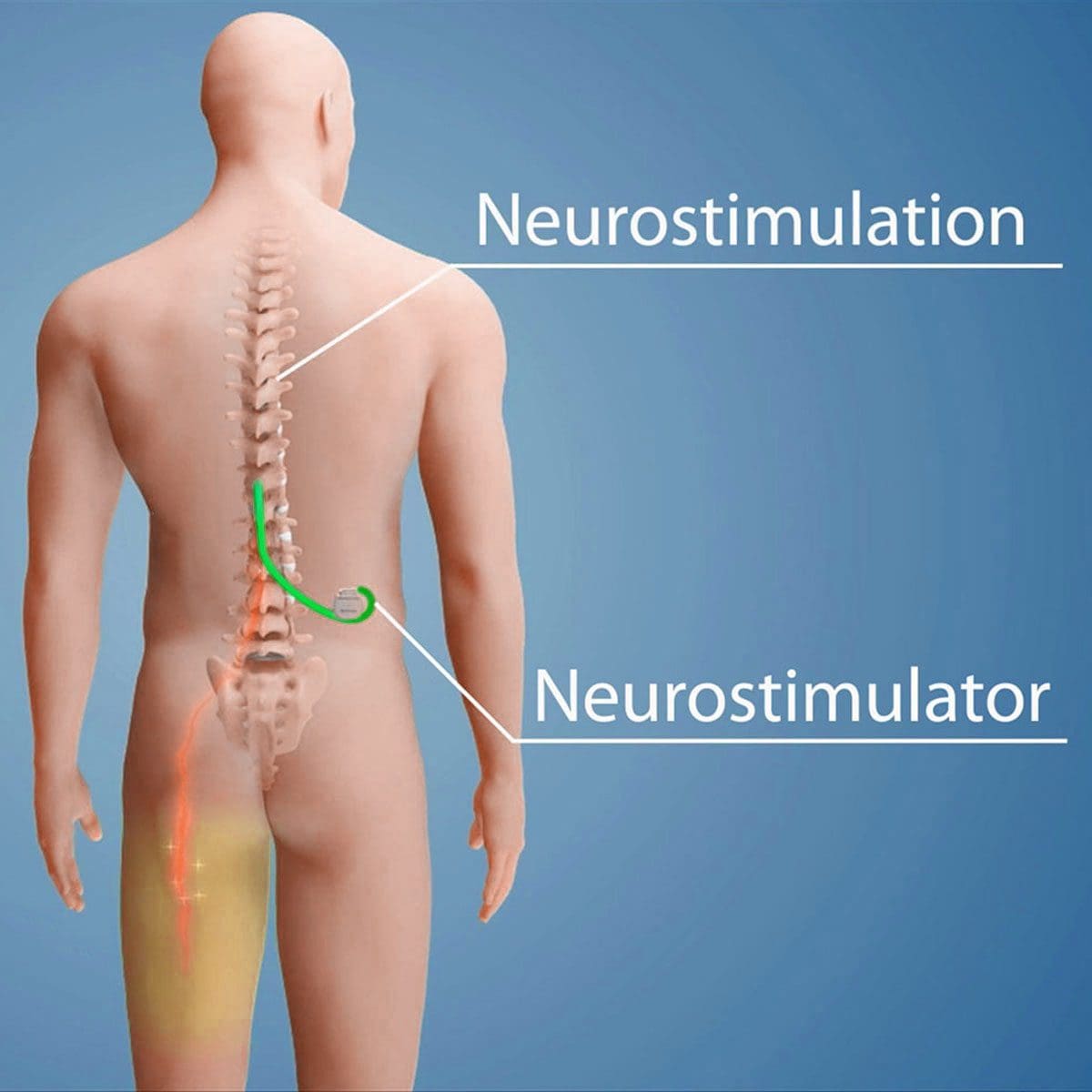
Neurostimulator:
This is the entire device that is implanted and sends out electrical impulses through a lead wire to the nerves in the spine.
Lead:
The thin wire delivers the electrical impulses from the neurostimulator.
Remote control:
This turns on/off the stimulator and increases or decreases the amount of stimulation.
Charger:
Stimulators are rechargeable and normally require recharging for about one hour every two weeks.
Â
Spinal Stimulator Types:
Â
Traditional stimulators
These produce a gentle ringing/tingling sensation that masks the pain.
Burst stimulators
These send out random interval bursts of electrical impulses designed to copy how the body sends out nerve impulses.
High-frequency stimulators
These reduce pain without generating tingling sensations. Â

Types of Pain Spinal Stimulation Treats
The U.S. FDA approves spinal stimulation to treat chronic back and leg pain, including pain that doesn’t go away after back surgery, known as failed back surgery syndrome. Chronic neuropathic back and leg pain are the most common types that stimulation treats. This means back or leg pain caused by nerve damage from:
- Auto accident
- Injury – personal, sports, work
- Disease
Acute pain is like stepping on a sharp piece of glass, where the pain serves as protection, letting you know something is wrong and not to continue. Whereas chronic neuropathic pain lasts for 3 months or more and does not help protect the body. Â
Spinal stimulation is also used to treat complex regional pain syndrome or CRPS. It is also used in treating peripheral neuropathic pain. This is a rare condition that affects the arms/hands or legs/feet and is believed to be caused by damage or malfunction of the nervous system. This is damage to the nerves outside of the spinal cord, often in the hands/feet, that is caused by an:
- Infection
- Trauma
- Surgery
- Diabetes
- Other unknown causes
Â
Appropriate Treatment
Spinal cord stimulation should not be used in pregnant patients, unable to operate the stimulation system, who went through a failed trial of spinal stimulation and are at risk for surgical complications. The decision to use spinal stimulation is based on an individual’s needs and risks. Talk to a doctor, spine specialist, chiropractor to see if spinal stimulation could be an option.
Â
Benefits and Risks
The effects of stimulation are different for everyone. Therefore, it is important to understand that spinal stimulation can help reduce pain but not eliminate it. Â

The Benefits of Spinal Cord Stimulation
In addition to reducing pain, other benefits of spinal stimulation include:
- Better sleep
- Improved body function
- Increased activity
- Improved mobility
- Reduced opioid medication/s use
- Less need for other types of pain meds
- Reduced dependence on braces/bracing
Â
Risks
During the implantation, there is a risk for:
- Bleeding
- Infection
- Pain at the site of incision
- Nerve damage
- Rarely paralysis

 For some individuals, scar tissue can build up over the electrode, blocking the stimulator’s electrical impulse. The lead wire could move or shift out of position. This could lead to impulses being sent to the wrong location. The device itself could shift under the skin, causing pain, making it hard to re-charge or communicate with the remote.
There is a risk that the lead wire could detach or break off, causing a malfunction and require a replacement. Also, individuals could respond well to the stimulation at first, but later on, they develop a tolerance, so the therapy no longer has the same impact. The pain could get worse because the nerves stop responding.
Â
Take Precautions
Discuss what you can and can’t do with a doctor, spine specialist, or chiropractor after the stimulator is implanted and activated. Here are a few precautions:
- Do not drive or operate heavy equipment when the stimulator is active.
- Stimulation systems could set off metal detectors, which could require manual screening.
MRIs, electrocautery, diathermy, defibrillators, and cardiac pacemakers could negatively interact with certain types of stimulators. This could result in injury or damage to the spinal stimulator. Talk to your doctor to determine if a spinal stimulator is a treatment option that will work for you.
Â
Weight Loss Techniques – Push Fitness Center
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Spinal Stimulation and Chronic Back Pain" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933







Comments are closed.