Venous Insufficiency: EP Personal Injury Doctors
Arteries carry blood from the heart to the rest of the body. The veins transport blood back to the heart, and the valves in the veins stop the blood from flowing backward. When the veins have difficulties sending blood from the limbs back to the heart, this is known as venous insufficiency. With this condition, the blood does not flow back properly to the heart, causing blood to accumulate in the veins of the legs. Chiropractic care, therapeutic massage, and functional medicine can increase and improve circulation and help manage symptoms.
Venous Insufficiency
The circulatory system is responsible for transporting blood, oxygen, and nutrients to the cells in the body. This system consists of the heart, arteries, veins, and capillaries. When blood circulation is restricted, it can lead to a buildup of toxins and waste products, which can cause various health problems, including fatigue, muscle cramps, and dizziness. Unhealthy circulation can also contribute to other health conditions like heart disease, stroke, and diabetes. The most common causes of venous insufficiency include:
- Blood clots
- Varicose veins
- A family history of venous insufficiency.
- Deep vein thrombosis.
- When forward flow through the veins is obstructed, such as in the case of a blood clot, blood builds up below the clot, which can lead to venous insufficiency.
- In varicose veins, the valves can be missing or damaged, and blood leaks back through the defective valves.
- In some cases, weakness in the leg muscles that push blood forward can also contribute to venous insufficiency.
- Venous insufficiency is more common in women than men and is more likely in adults over 50.
Circulation Symptoms
There are different symptoms associated with unhealthy circulation, and can include:
- Tingling or numbness in the extremities
- Cold hands and feet
- Pain or cramping in the muscles
- Weakness or fatigue
- Dizziness or lightheadedness
- Nausea
- Shortness of breath
- Erectile dysfunction
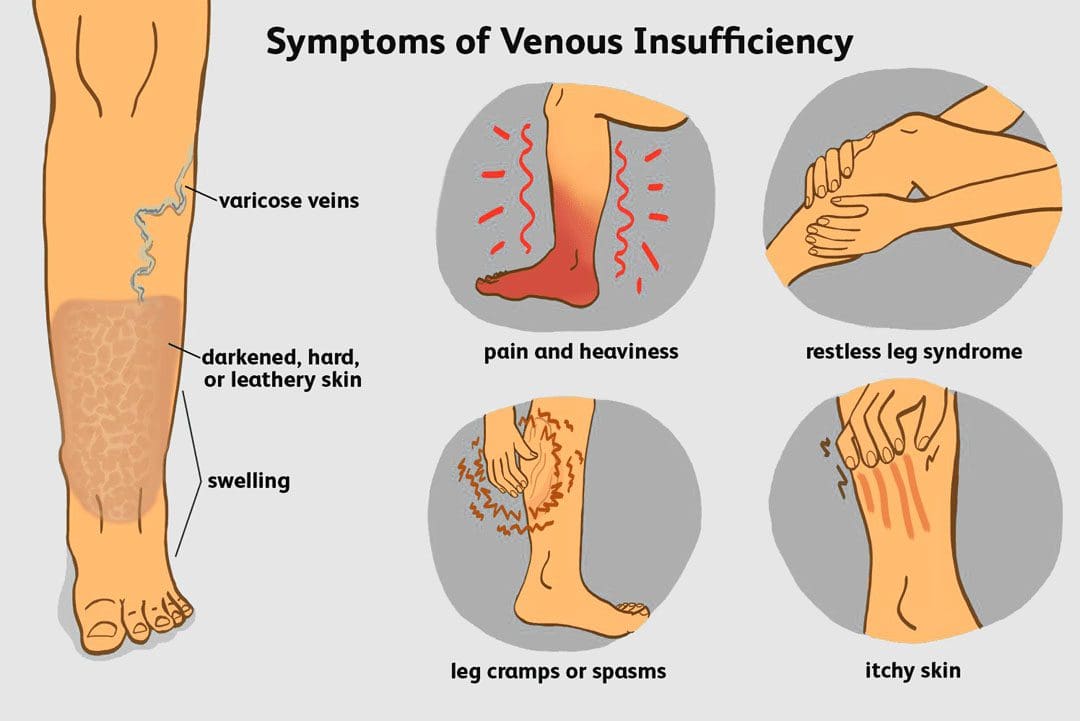
Symptoms of venous insufficiency include:
- Swelling of the legs or ankles – edema
- Pain that gets worse when standing and improves when raising the legs.
- Aching, throbbing, or a feeling of heaviness in the legs.
- A sense of tightness in the calves.
- Leg cramps
- Weak legs
- Itchy legs
- Thickening of the skin on the legs or ankles.
- Skin that is changing color, especially around the ankles
- Varicose veins
- Leg ulcers
Diagnosis
A doctor will perform a physical examination and take a complete medical history. They may order imaging tests to locate the source of the problem. These tests may include a venogram or a duplex ultrasound.
Venogram
- A doctor will insert an intravenous contrast dye into the veins.
- Contrast dye causes the blood vessels to appear opaque on the X-ray image, which helps the doctor see them on the image.
- This dye will give the doctor a clear image of the blood vessels.
Duplex Ultrasound
- A duplex ultrasound tests the speed and direction of blood circulation in the veins.
- A technician will place gel on the skin and press a small hand-held instrument on and around the area.
- The instrument uses sound waves that bounce back to a computer and produce images of blood circulation.
Treatment
Treatment will depend on various factors, including the reason for the condition and individual health status and history. Other factors a doctor will consider include:
- Specific symptoms
- Age
- The severity of the condition
- Medication and/or procedure tolerance
The most common treatment is prescription compression stockings.
- These special stockings apply pressure on the ankle and lower leg.
- They help improve blood circulation and reduce leg swelling.
- Compression stockings come in a range of prescription strengths and lengths.
Strategies
Treatments can include several methods.
Improving Circulation
Chiropractic adjustments and vascular massage therapy on the legs can help improve blood circulation. Massage therapies such as vascular and lymphatic drainage massages aim to increase circulation, improve tissue nutrition, and can benefit patients with varicose veins and chronic venous insufficiency.
- The technique for lymphatic drainage involves light strokes to move lymph fluid into lymph vessels.
- The technique used to improve circulation involves short strokes to move blood from the valves to the veins.
However, massage therapy is not for all patients with vein diseases and conditions.
- Massage therapy is not recommended for patients with advanced-stage vein disease, in which large and bulging veins, ulcerations, and discoloration are present.
- Massaging the area could cause the weakened veins to burst, worsening the condition.
- Massage therapy is also unsafe for patients with deep vein thrombosis (DVT), as it could dislodge a clot and cause it to travel.
Medications
Medications may be prescribed. These include:
- Diuretics – medications that draw extra fluid from the body and are excreted through the kidneys.
- Anticoagulants – medicines that thin the blood.
- Pentoxifylline – medicine that helps improve blood circulation.
Surgery
More serious cases may require surgery. A doctor may suggest one of the following surgical procedures:
- Surgical repair of the veins or valves.
- Removing the damaged vein.
- Minimally invasive endoscopic surgery – The surgeon inserts a thin tube with a camera to see and tie off damaged veins.
- Laser surgery – A treatment that uses laser light to fade or close off damaged veins.
- Vein bypass – A healthy vein is transplanted from a different body area. Generally used only in the upper thigh and as a last option for severe cases.
Venous Insufficiency: What You Need To Know
References
Annamaraju P, Baradhi KM. Pentoxifylline. [Updated 2022 Sep 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559096/
Chronic venous insufficiency. (n.d.). hopkinsmedicine.org/healthlibrary/conditions/cardiovascular_diseases/chronic_venous_insufficiency_85,P08250/
Evrard-Bras, M et al. “Drainage lymphatique manuel” [Manual lymphatic drainage]. La Revue du praticien vol. 50,11 (2000): 1199-203.
FIELDS, A. “Leg cramps.” California medicine vol. 92,3 (1960): 204-6.
Felty, Cindy L, and Thom W Rooke. “Compression therapy for chronic venous insufficiency.” Seminars in vascular surgery vol. 18,1 (2005): 36-40. doi:10.1053/j.semvascsurg.2004.12.010
Mayo Clinic Staff. (2017). Varicose veins.mayoclinic.org/diseases-conditions/varicose-veins/diagnosis-treatment/drc-20350649
Patel SK, Surowiec SM. Venous Insufficiency. [Updated 2022 Aug 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430975/
Youn, Young Jin, and Juyong Lee. “Chronic venous insufficiency and varicose veins of the lower extremities.” The Korean journal of internal medicine vol. 34,2 (2019): 269-283. doi:10.3904/kjim.2018.230
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Venous Insufficiency: EP Personal Injury Doctors" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card








Comments are closed.