Cauda Equina Syndrome Nerve Compression Chiropractic Diagnosis
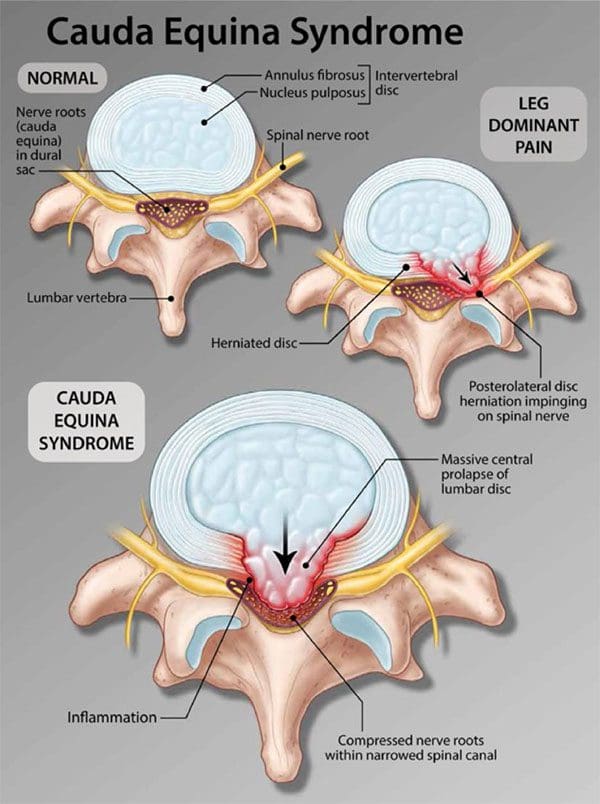
Cauda Equina Syndrome
The term comes from Latin that means horse’s tail. The cauda equina forms the group of nerves that run through the lumbar spinal canal. Generally, the condition means two things:- There is nerve compression of most of the lumbar spinal canal
- Compression symptoms like numbness or weakness in the leg/s
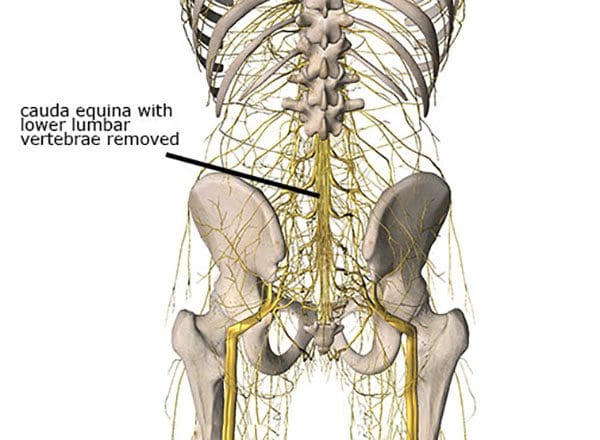
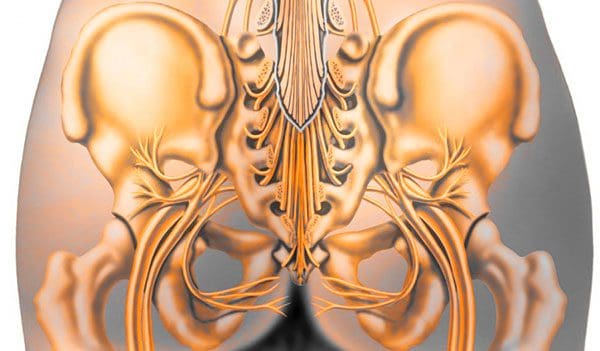
Sneaky Presentation
One of the major factors is long-term compression that individuals do not realize they have. Individuals are more likely to be aware of symptoms from another spinal condition before cauda equina syndrome presents. However, the condition presents quickly but often other overlapping back problems mask cauda equina syndrome.Causes
The syndrome can be brought on from anything that compresses the nerves. Most commonly, it is a root compression from degenerative processes, specifically lumbar disc herniations. Other causes include:- Bleeding like an epidural hematoma
- Trauma like fractures or penetrating trauma
- Tumors growing in the canal or the collapse of a tumor-affected bone
- Disc herniations can progressively grow in size, which leads to a slowly-evolving cauda equina syndrome.
- An enlarging disc herniation or synovial cyst can further compromise the already compressed nerves.
- Overgrowth of arthritic joints or bone spurs into the spinal canal can lead to long-term compression.
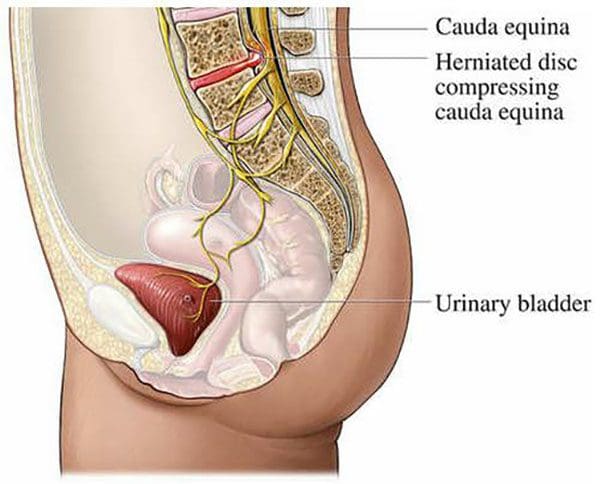
Symptoms
- Back pain
- Leg pain
- Sciatica
- Saddle numbness that extends into other areas of the legs
- Neurogenic bladder dysfunction. This can range from difficulty starting to urinate or limited and/or non-voluntary control urinating.
- Bowel dysfunction
- Sexual dysfunction
Diagnosis
A doctor will examine any significant changes in bladder, bowel, or leg function that are considered red flags prompting an early and complete assessment. A physician will ask for a complete/detailed history of the onset and progression of symptoms. The second is a close physical examination which includes testing sensation and strength along with a rectal exam to assess voluntary contraction. Also checking the body’s reflexes, assess walking gait and alignment. If most or all of the symptoms are presenting this will set in motion spinal imaging or an MRI. If the symptoms, exam, and imaging match, it will lead to an emergency admission to the hospital.
Body Composition Spotlight
Obesity and Osteoarthritis Connection
A variety of factors contribute to the development of osteoarthritis, including genetic factors and lifestyle choices. Research supports obesity is a significant risk factor in the development of osteoarthritis. It is pretty straightforward as body weight increases this equals increased load on the spine, and joints, especially the weight-bearing ones like the hips and knees. Increased pressure leads to early wearing, tearing, and eventual development of osteoarthritis. Added weight affects the body’s biomechanics and gait patterns. However, obesity has also been shown to be a risk factor even on the non-weight-bearing joints. This is based on adipose tissue, which is more than just insulation. Adipose tissue is metabolically active and is involved in the secreting adipokines and cytokines which promote an inflammatory response. Pro-inflammatory adipokines and cytokines can have detrimental effects on joint tissue including damage to cartilage, synovial joints, and subchondral bone. The effect of inflammation on the joints in the body can contribute to the development of osteoarthritis.Dr. Alex Jimenez’s Blog Post Disclaimer
The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*References
Causes of Cauda Equina: Neurosurgical Focus. (June 2004) “Spinal epidural hematoma causing acute cauda equina syndromeâ€Â https://pubmed.ncbi.nlm.nih.gov/15202871/ Arriving at a Diagnosis: British Journal of Neurosurgery. (August 2010) “Reliability of clinical assessment in diagnosing cauda equina syndromeâ€Â https://www.tandfonline.com/doi/abs/10.3109/02688697.2010.505987Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Cauda Equina Syndrome Nerve Compression Chiropractic Diagnosis" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933








Comments are closed.