Patellar tendinitis is a health problem characterized by the inflammation of the tendon which combines the kneecap, or patella, to the shinbone. The knee pain may range from mild to severe depending on the conditions of the knee injury.
Patellar tendinitis and knee injuries can occur due to automobile accidents although it is most commonly a sports injury among athletes who play at volleyball and basketball, known as
Causes of Patellar Tendinitis
Patellar tendinitis is caused by strain on the knee frequently from overuse in bodily pursuits. Stress can create tears along the tendons which can cause inflammation in the complex constructions of the knee.
Contributing factors of patellar tendinitis include:
- Tight or stiff leg muscles
- Uneven leg muscle strength
- Toes, ankles, and legs
- Obesity
- Sneakers without cushioning that is enough
- Tough playing surfaces
- Chronic health issues that weaken the tendon
Athletes have a higher chance of developing patellar tendinitis because jumping, jogging, and squatting put force over the thoracic. Running can place a force of as many as five times the body weight on the knees.
Physical activity for a protracted amount of time has been formerly associated with jumper’s knee. A 2014 research study noted that jump frequency was also an important risk factor for players.
Indicators of Patellar Tendinitis
Patellar tendinitis’ symptoms include soreness, discomfort, and tenderness at the base of the kneecap or patella. Other indicators of patellar tendinitis may include a burning feeling. For many patients, kneeling down or getting up from a squat is also particularly debilitating.
The pain associated with patellar tendinitis may be irregular at first, manifesting after participating in activities that are physical. Injury or damage to the tendon can also make the pain worse. Jumper’s knee may affect regular daily activities, such as climbing stairs or sitting in a vehicle.

Patellar tendinitis is a particularly common source of pain and discomfort in the patellar area of many individuals. Research studies have shown that patellar tendinitis could be associated with sprains and stiff ankle movements, among other sports injuries, while it happens as a consequence of constant or repetitive jumping, although it may develop due to damage or injury from an automobile accident.
Dr. Alex Jimenez D.C., C.C.S.T. Insight
Patellar Tendinitis Diagnosis
At the beginning of a consultation, the medical professional will initially ask the patient about their particular health issue. The doctor will physically evaluate the patient’s knee probe for where they’re feeling pain, and also examine the assortment of knee motion by extending and bending the patient’s leg.
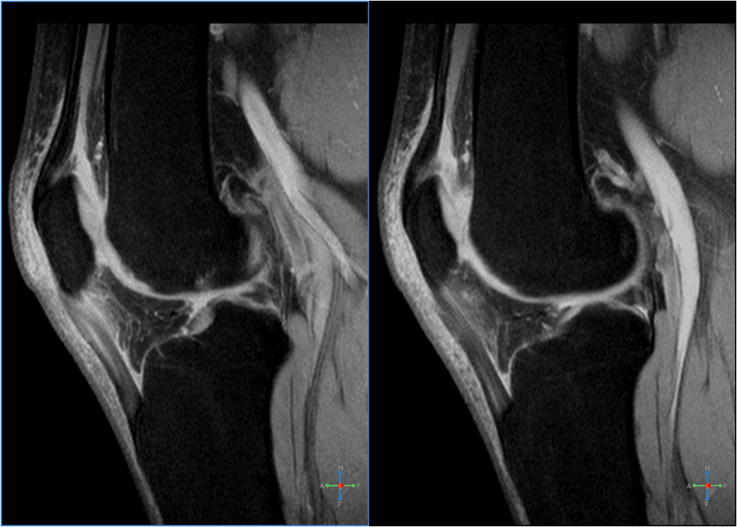
Furthermore, the healthcare professional may ask for imaging diagnostics to find out if there’s injury or any damage to the tendon or perhaps the bone. These tests will help rule out a broken bone, or fracture. The health care provider may use an X-ray to search for a fractured or displaced kneecap, and an MRI or an ultrasound to reveal any injury to the tissue.
Patellar Tendinitis Treatment
Drugs and/or Medicines
The healthcare practitioner may prescribe medication that are over-the-counter and/or medications for pain relief and inflammation reduction.
These can include:
- Ibuprofen (Advil)
- Naproxen sodium (Aleve)
- Acetaminophen (Tylenol)
The medical professional may recommend using corticosteroid injection in the region around the patellar tendon if the individual’s symptoms are severe. This therapy is effective in reducing acute pain.
Another method of treatment utilizes an electric charge to push it through the skin and then corticosteroid by spreading the medicine for patellar tendinitis in a process called iontophoresis.
Chiropractic Care and Physical Therapy
The goal of chiropractic care and physical therapy for patellar tendinitis is to reduce pain and inflammation, among other symptoms, as well as to strengthen the leg and thigh muscles together with stretches and exercises.
Even while resting, then the physician may recommend that you wear a brace and use crutches to avoid damage or harm to the tendon, if the patient’s symptoms are severe. Then they can start participating in physical treatment activities if the patient has no debilitating symptoms.
A rehab program includes:
- A warm-up interval
- Massage, heat or ice to the knee
- Stretching exercises
- Strengthening exercises
A doctor of chiropractic, or chiropractor, may use ultrasound and electrical stimulation to ease the patient’s knee pain. A knee brace may also help reduce pain when engaging in physical activities. A workout program that might include a set of exercises and stretches may be developed by the medical professional.
Surgery
When other therapies aren’t effective in relieving symptoms, the physician may advise surgery to repair the patellar tendon. Traditional surgery involves opening the knee to scratch on the kneecap and tendon. More lately, arthroscopic operation is utilized for this particular process. This surgical intervention entails making four small incisions in the knee and it has a shorter healing time.
The healing period for operation varies per process. Some intervention advice involves using a cast for immobilization. AÂ rehab program is suggested by others. Irrespective of the level of damage and/or harm, it is vital for individuals to seek medical attention due to their patellar tendinitis. The scope of our information is limited to chiropractic as well as to spinal injuries and conditions. To discuss the subject matter, please feel free to ask Dr. Jimenez or contact us atÂ
Curated by Dr. Alex Jimenez

Additional Topic Discussion: Relieving Knee Pain without Surgery
Knee pain is a well-known symptom which can occur due to a variety of knee injuries and/or conditions, including sports injuries. The knee is one of the most complex joints in the human body as it is made-up of the intersection of four bones, four ligaments, various tendons, two menisci, and cartilage. According to the American Academy of Family Physicians, the most common causes of knee pain include patellar subluxation, patellar tendinitis or jumper’s knee, and Osgood-Schlatter disease. Although knee pain is most likely to occur in people over 60 years old, knee pain can also occur in children and adolescents. Knee pain can be treated at home following the RICE methods, however, severe knee injuries may require immediate medical attention, including chiropractic care.

EXTRA EXTRA | IMPORTANT TOPIC: Knee Injury Treatment
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Patellar Tendinitis After Automobile Accidents" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933







Comments are closed.