Previous study reported by SIB suggested that fluoroquinolone antibiotics can introduce a potential threat to tendon health in sportsmen and women. Chiropractor, Dr. Alexander Jimenez looks at more recent research on fluoroquinolones and explores the implications for clinicians.
The development of antibiotics is without doubt among mankind’s greatest scientific accomplishments, saving countless millions of lives since their introduction. However, notwithstanding the current concerns about ‘superbug’ resistance, not everything is rosy in the antibiotic garden. A few decades back, we reported growing signs that one group of antibiotics — fluoroquinolones — might be implicated in rapid-onset tendon degeneration, demonstrating sportsmen and women to an increased risk of tendonitis or even tendon rupture. In the intervening years, more research into this subject was carried out, providing a helpful insight to clinicians dealing with athletes who may have athletes in their care that are either taking or have taken fluoroquinolone antibiotics.
Fluoroquinolone Anatomy
Fluoroquinolones are successful, wide- Spectrum antibiotics first developed in the 1970s, which play an important part in the therapy of severe bacterial infections such as pneumonia, typhoid, diarrhea, kidney/urinary tract diseases and many other stubborn and virulent infections. Indeed, some of the newer iterations of fluoroquinolones are especially effective against bacteria such as Staphylococcus Aureus and Staphylococcus Pneumoniae, which are very resistant to several other antibiotics.
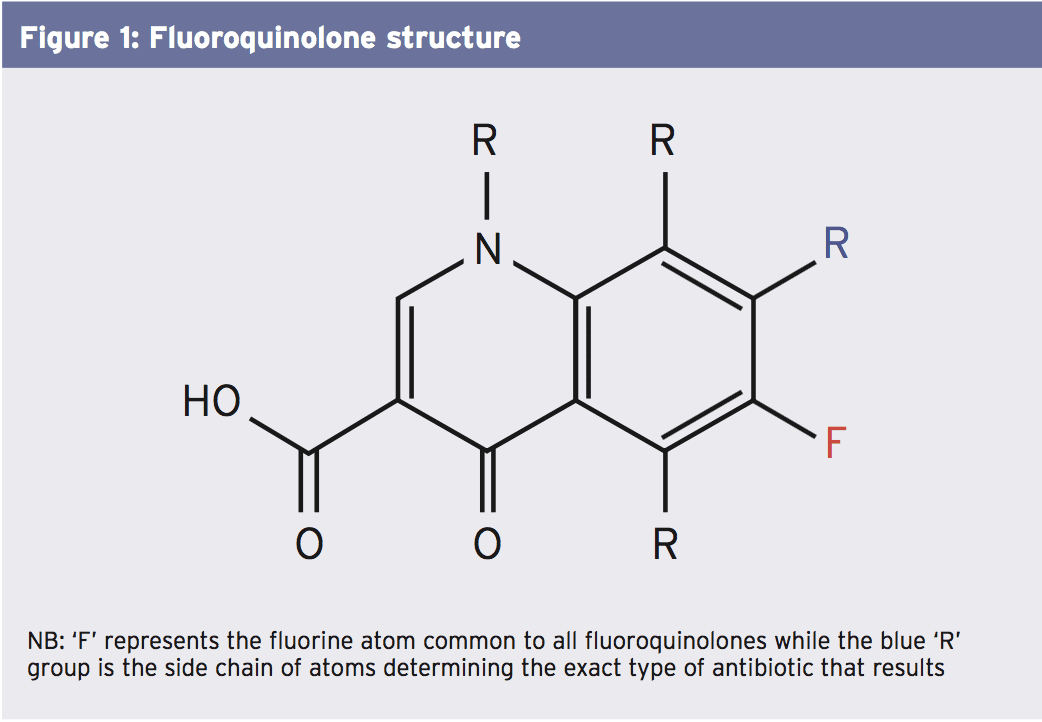
The fluoroquinolones (see Figure 1) are a subgroup of the larger quinolone family of antibiotics. All quinolones work by preventing bacterial DNA from unwinding and duplicating. Examples of commonly used fluoroquinolone antibiotics include ciprofloxacin, levofloxacin, norfloxacin and gemifloxacin.All the fluoroquinolones share the exact same necessary chemical structure (shown in Figure 1 below). The ‘F’ describes the fluorine atom (giving rise to this ‘fluoro’ in fluoroquinolones), while the ‘R’ describes the compound side set — it is the different R groups that produce the various types of fluoroquinolone antibiotics.
 Fluoroquinolone Factors
Fluoroquinolone Factors
Hailed by some as ‘wonder antibiotics’, fluoroquinolone use by physicians Increased dramatically towards the turn of the century. In the late 90s nevertheless, evidence began to emerge linking fluoroquinolone antibiotic usage with structural changes in the cellular level to connective tissue in the body — particularly to collagen, an important and vital part of tendon tissue.
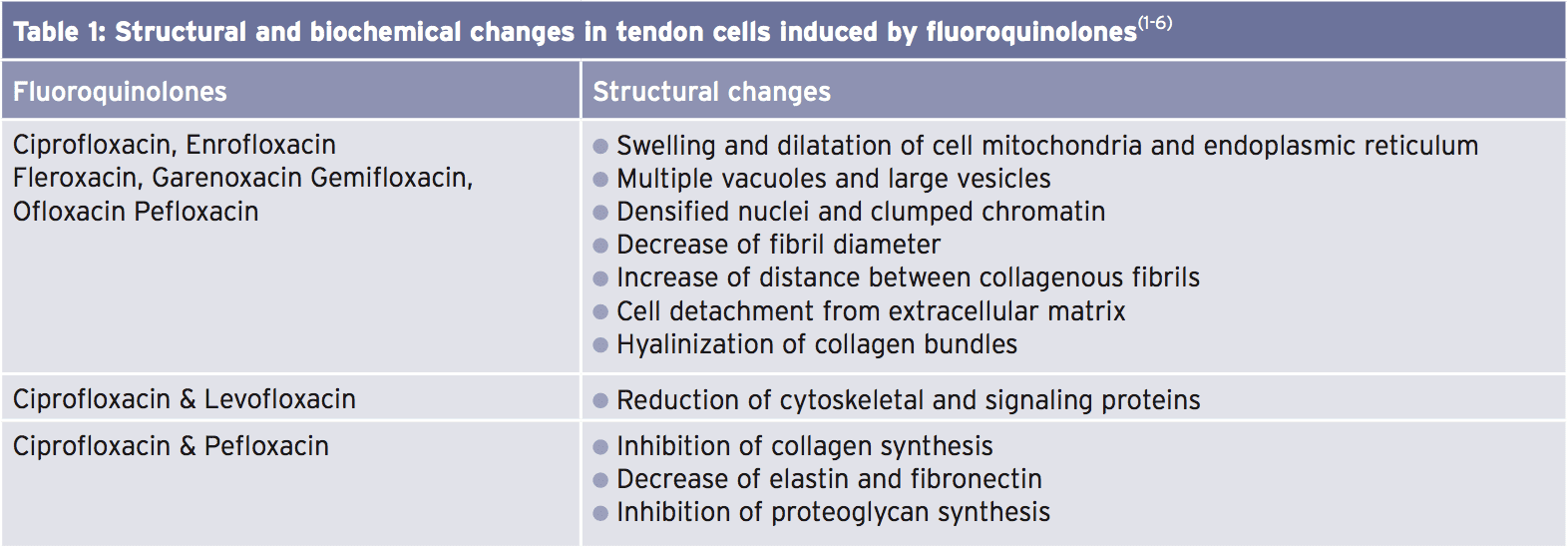
A number of the first findings came about as a consequence of studies on mice (see Table 1)(1-6). However, studies on human cell trials appeared to signal that by inducing a decrease in essential elements of tendon tissue like collagen type I, collagen, fibronectin and proteoglycan, fluoroquinolone-induced degenerative structural modifications to tendon tissue were also possible in human tendon tissue(7).
 Around about the exact same time, a growing number of tendonitis and tendon rupture cases were being observed among patients taking fluoroquinolone antibiotics. A 2003 Canadian study of 98 case studies from the scientific literature found that pefloxacin and ciprofloxacin were most often implicated, but tendon injury was documented with most fluoroquinolones(8). The median duration of fluoroquinolone therapy before the beginning of tendon injury was eight days, although symptoms occurred as early as two hours after the first dose and as late as six months after therapy was discontinued. Up to one-half of patients experienced shortness rupture, and of them, nearly one third had also received long-term corticosteroid treatment before or during fluoroquinolone use.
Around about the exact same time, a growing number of tendonitis and tendon rupture cases were being observed among patients taking fluoroquinolone antibiotics. A 2003 Canadian study of 98 case studies from the scientific literature found that pefloxacin and ciprofloxacin were most often implicated, but tendon injury was documented with most fluoroquinolones(8). The median duration of fluoroquinolone therapy before the beginning of tendon injury was eight days, although symptoms occurred as early as two hours after the first dose and as late as six months after therapy was discontinued. Up to one-half of patients experienced shortness rupture, and of them, nearly one third had also received long-term corticosteroid treatment before or during fluoroquinolone use.
As concern over the association between Fluoroquinolone use and tendonitis/tendon rupture grew, the US FDA issued a ‘hardened warning’ followed in 2008 with a more general alert to the dangers of fluoroquinolone use stating(9): “Tendinitis and tendon rupture most often involves the Achilles tendon, and rupture of the Achilles tendon may require surgical repair. Tendinitis and tendon rupture from the rotator cuff, the hand, the biceps, and the thumb also have been reported. Tendon rupture can occur during or following completion of fluoroquinolone usage; instances happening to several months following completion of treatment have been reported. Fluoroquinolones should be discontinued if the patient experiences pain or inflammation in a tendon (symptoms which may precede rupture of the tendon), or tendon rupture. Patients are advised, at the first sign of tendon irritation, swelling, or inflammation, to stop taking the fluoroquinolone, to prevent exercise and use of the affected area, and to promptly contact their healthcare provider about switching to a non-fluoroquinolone antimicrobial drug.”
 Recent Evidence
Recent Evidence
What does the science say about fluoroquinolone use and tendinopathy/ rupture? Concerning aetiology, compelling evidence suggests that fluoroquinolones can quickly affect the chemical composition of tendon construction by depleting amounts of glycosaminoglycans (GAGs — compounds critical to the elasticity and integrity of structural tissue) in the tendon.
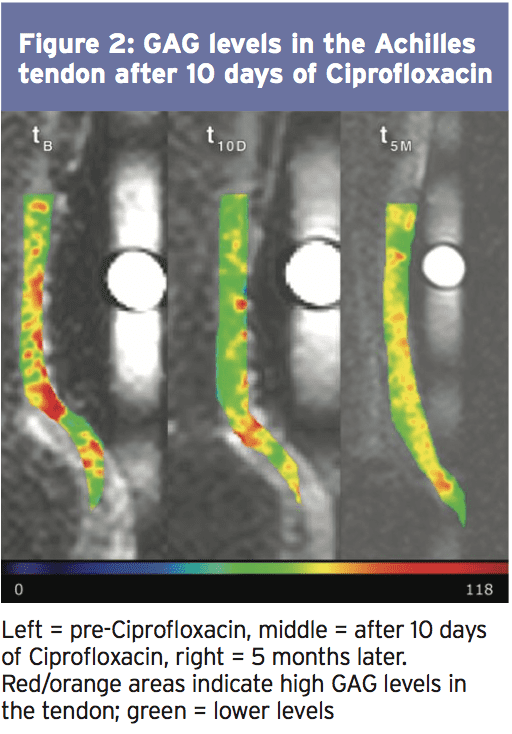
In a study released earlier this year, researchers used a technique called sodium magnetic resonance imaging (sodium MR) to study pathological changes and changes in GAG degrees in the Achilles tendons in the 14 ankles of 7 men who took 500ms of Ciprofloxacin twice a day for 10 days(11). As figure 2 shows, after 10 days, there was a marked reduction in the GAG content of the Achilles tendon, which though reversible, still hadn’t fully recovered 5 months after ending the Ciprofloxacin program.
 The prolonged period of interrupted tendon pathology after fluoroquinolone administration may be aggravated by diminished tendon healing capacity. A recent study on mice appeared at tendon healing capability in those treated using Fleroxacin before rotator cuff surgery(12). In contrast to control mice that received no Fleroxacin, the treated mice showed considerably less fibrocartilage and poorly organized collagen in the healing enthesis. Moreover, the treated mice had a significantly reduced tendon cross-sectional area and the researchers reasoned that the fluoroquinolone therapy had negatively influenced tendon healing, which would have implications for patients undergoing tendon surgery/repair in the months following a course of fluoroquinolones.
The prolonged period of interrupted tendon pathology after fluoroquinolone administration may be aggravated by diminished tendon healing capacity. A recent study on mice appeared at tendon healing capability in those treated using Fleroxacin before rotator cuff surgery(12). In contrast to control mice that received no Fleroxacin, the treated mice showed considerably less fibrocartilage and poorly organized collagen in the healing enthesis. Moreover, the treated mice had a significantly reduced tendon cross-sectional area and the researchers reasoned that the fluoroquinolone therapy had negatively influenced tendon healing, which would have implications for patients undergoing tendon surgery/repair in the months following a course of fluoroquinolones.
Recent Risk Data
Concerning the risk of specific Fluoroquinolone drugs, recent research has indicated that Ciprofloxacin, Fleroxacin, Pefloxacin and Ofloxacin present the greatest danger to tendon health(13). While other fluoroquinolones such as Trovafloxacin and Levofloxacin may present less of a risk, they’re not risk free. For instance, Levofloxacin has been implicated in Achilles tendon rupture in some case studies(14), while for other fluoroquinolones, there may simply not be enough information to determine safety one way or the other.
More worryingly is the recent evidence suggests that when it comes to tendonitis or tendon rupture, athletes and fitness enthusiasts may be especially vulnerable to the consequences of fluoroquinolones. There are a range of explanations for why this is how it is. Firstly, excessive loading of joints during physical training is considered a major pathologic stimulus for tendon degeneration. This is because exercise increases the production of enzymes known as amatrix metalloproteinases’, a few of which could adversely alter the structure of the extracellular matrix of tendons(15).
In addition, we know that low-dose Corticosteroids in isolation may increase the risk of Achilles tendon rupture, and evidence suggests that combined use of corticosteroids using fluoroquinolones potentiates this adverse effect(16,17). Indeed, studies indicate that over 50\% of patients with fluoroquinolone-related tendon rupture had received systemic or inhaled corticosteroids(18), which patients prescribed both fluoroquinolones and corticosteroids have a 46-fold greater risk of Achilles tendon rupture than people taking neither drugs(19)!
Given these facts, a recent review of Fluoroquinolone use among athletes has indicated that athletes should not be prescribed fluoroquinolones and ought to be given alternative antibiotics whenever possible(20). This is particularly true in the light of the added risk of corticosteroid treatment; asthma is common among sportsmen and women(21), lots of whom might be using corticosteroid medication. Fluoroquinolone use in these athletes could consequently be very hazardous.
When fluoroquinolone antibiotics are the only solution for the athlete, there’s some evidence from cell culture studies that the co-ingestion of vitamin E might help relieve some of the damaging effects(22,23). This might occur due to the ability of vitamin E to help avoid of free-radical damage in biological membranes.
But if this protective effect is significant in humans undergoing fluoroquinolone therapy is unknown and also the best choice by far is to get athletes to steer clear of fluoroquinolones altogether when possible.
Rehab & Fluoroquinolone – Induced Tendinopathy
Graduated eccentric training regimes, in that muscle tendons are subjected to growing loads during muscle elongation, have proved both popular and effective for treatment and rehabilitation of tendinopathy — and that this approach is supported by the literature(24). For sportsmen and women, bizarre training programs have been proven to be particularly successful, leading to a success rate of approximately 90\% in those with tendinopathy(25) — a significantly better result than for the (more sedentary) population as a whole(26).
However, while loading tendon with eccentric exercise may be suitable for healing tendinopathy most athletes, that this strategy shouldn’t be utilized for healing fluoroquinolone-induced tendon conditions, at least at the early stages of symptoms. In study on this issue, Greene demonstrated that patients with fluoroquinolone-related tendinopathy ought to be rehabilitated using a 2-phase approach (see Box 2)(27):

- An initial phase of bracing and support to enable the tendon to recoup from the chemical injury brought on by the fluoroquinolone
- A second stage, consisting of progressive loading
Summary & Recommendations
Evidence continues to mount suggesting that fluoroquinolone antibiotics have been harmful for sportsmen and women, who appear particularly vulnerable for their effects. Not only do they adversely affect the chemical composition and structural Integrity of tendons, their usage seems to inhibit the normal repair mechanisms that bring about recovery from tendon injury. Worse, the danger of fluoroquinolone- Induced tendinopathy is further raised when corticosteroid medicine is being used, which is the case in several athletes With asthmatic conditions. In the light of the above, clinicians should follow the recommendations below when coping with athletes that are or who have from the past 6 months been on fluoroquinolone antibiotics.

Legal Notice: The above article though out of clinical scope in Texas, was not intended to give advice in any way. The intention is to provide awareness on physiological implications certain medications may have on musculoskeletal tissue integrity as it pertains to healing and repair.
References
1. Toxicology 2005, 212, 24-36
2. Int. J. Antimi- crob. Agents 2010, 35, 366-374
3. Antimicrob. Agents Chemother. 2000, 44, 261-266
4. Arch. Toxicol. 2001, 75, 97-102
5. Arch. Toxicol. 2001, 75, 369-374
6. Arch. Toxicol. 2003, 77, 521-526
7. Am. J. Sports Med. 2000, 28, 364-369
8. Clin Infect Dis. 2003 Jun 1;36(11):1404-10
9. US FDA Alert: 7/8/2008 – http://www.fda.gov/drugs/drugsafety/postmarketdrugsafety informationforpatientsandproviders/ucm126085.htm
10. J Clin Aesthet Dermatol. 2010 April; 3(4): 49–54
11. Radiology. 2015 Jun; 275(3): 763–771
12. Am J Sports Med. 2014 Dec;42(12):2851-9
13. Biomed Semantics. 2015 May 1;6:18.
14. Foot Ankle Int. 2007;28(12):1287–1289; Chemotherapy. 2007;53(2):85–103
15. Br J Sports Med. 2005;39(11):789–791
16. BMJ Case Rep. 2009;2009. doi:10.1136/bcr.08. 2008.0697
17. J Plast Reconstr Aesthet Surg. 2008;61(7):830–834
18. Clin Infect Dis. 2003;36(11):1404–1410
19. Drug Saf. 2006;29(10):889–896
20. J Athl Train 2014;49(3):422–427
21. Dan Med J. 2012;59(4):A4405
22. BMC Pharmacol. 2008 Feb 11;8:2. doi:10.1186/1471-2210-8-2
23. Hum Exp Toxicol. 2002;21(12):635–641
24. Sports Med Arthrosc Rev. 2000;8(1):17–31
25. Sports Traumatol Arthrosc. 2003;11(5):327–333
26. J Med Sci Sport. 2007;10(1):52–58
27. Phys Ther. 2002;82(12):1224–1231
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Fluoroquinolones Antibiotics & Injury" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933



 Recent Evidence
Recent Evidence




Comments are closed.