Neck pain that is not caused by whiplash or other trauma has a postural component as part of the underlying problem. Sitting atop the body, the health of the neck is subject to the  curvature of the spine below and the position of the head above.
See Chronic Neck Pain: What Condition Is Causing My Neck Pain?
The neck muscle pain can be caused by the following neck muscles becoming tight:
- Scalene muscles (three pairs of muscles that help rotate the neck)
- Suboccipital muscles (four pairs of muscles used to rotate the head)
- Pectoralis minor muscles (a pair of thin triangular muscles at the upper part of the chest)
- Subscapularis muscles (a pair of large triangular muscles near each shoulder joint)
Levator scapulae muscles (a pair of muscles located at the back and side of the neck).If the alignment of the head and spine is not optimal, the neck can be predisposed to injury and/or the degenerative effects of wear and tear over time.
Forward Head & Shoulder Posture
The most common condition that contributes to neck pain is forward head and shoulder posture.
Forward head posture is when the neck slants forward placing the head in front of the shoulders.
This head position leads to several problems:
The forward pull of the weight of the head puts undue stress on the vertebrae of the lower  neck, contributing to degenerative disc disease and other degenerative neck problems.
Similarly, this posture causes the muscles of the upper back to continually overwork to counterbalance the pull of gravity on the forward head.
This position is often accompanied by forward shoulders and a rounded upper back, which not only feeds into the neck problem but can also cause shoulder pain.
The more time spent with a forward head posture, Â the more likely it is that one will develop neck and shoulder problems.
Workplace Ergonomics & Neck Pain
Poor Posture Effects On the Lower Cervical Vertebrae
The part of the neck that is particularly vulnerable to forward head posture is the lower part of the neck, just above the shoulders.
The lower cervical vertebrae (C5 and C6) may slightly slide or shear forward relative to one another as a result of the persistent pull of gravity on a forward head. This shear force can be a problem for patients with jobs that require them to look down or forward all day, such as pharmacists who spend many hours counting pills or data entry workers who look at a computer screen.
See Ergonomics of the Office and Workplace: An Overview
Long-Term Effects of Poor Posture
Prolonged shearing of the vertebrae from forward head posture eventually irritates the small facet joints in the neck as well as the ligaments and soft tissues.
This irritation can result in neck pain that radiates down to the shoulder blades and upper back, potentially causing a variety of conditions, including:
Trigger points in the muscles, which are points of exquisite tenderness that are painful to touch, along with limited range of motion
Disc degeneration problems, which may potentially lead to cervical degenerative disc disease, cervical osteoarthritis, or a cervical herniated disc.
BRAIN BASED POSTURAL CORRECTION

The neurologic system controls and coordinates all other systems of the body? What system provides the physical framework for all other systems of the body to resist gravity and function within our environment? The Posture System. These intricate systems work together to control and coordinate all experiences and actions throughout our lives.
Postural Neurology is defined as the network of neural impulses to support proper functional alignment of the Posture System. The purpose of Postural Neurology is to develop plasticity of proper structural alignment through brain based treatment protocols.
Why implement Postural Neurology into your practice? Quite simply, every musculoskeletal problem is at some level a neurologic problem. Neurology dictates movement, structure, and the function of your Posture System, overseeing and refining every single movement that you do on a daily basis.
It is an outdated system of healthcare to look at one part of the body, the site of injury or pain, and make assumptions about that person’s health and ability to function.
Identifying the area of injured tissue, then creating a rehabilitation plan around that injuryis less than adequate. The new system is all about function and whole posture patterns.
Segmental Rehabilitation & Brain Based Postural Correction
If the patient says “I hurt here,†or you test a weak muscle “here.†It does not mean that the problem lives “here.†This is simply information telling us that there is pain or dysfunction that is being expressed in that end organ. There is absolutely no indication that the problem is in that tissue. The noxious stimulus being interpreted by the brain is nothing more than a sensory input. The weak muscular output is nothing more than an insufficient motor plan.
This is the difference between segmental and brain based thinking. Segmental healthcare professionals do not see beyond the “hurt†or “weak†segment, oblivious to compensation patterns that are dampening function in the rest of the body.
Compartmentalized thinking is not adequate for a system as dynamically developed and as functionally managed as the human body. It simply won’t cut it.
This guide introduces you to the Neurology of the Posture System, so you can understand the functional output of the brain and how it contributes to upright postural design.
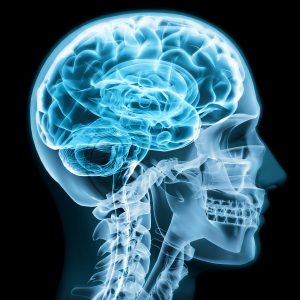
Motor Cortex:
The primary motor cortex is located in the frontal lobe of the brain.
The frontal lobe is the center of human development including executive decision-making, language, and problem-solving.
Located within the Motor cortex is the Motor Homonculus. The Motor Homonculus is a map of motor output for each part of your human anatomy. Within this map, the amount of cortex devoted to any given body region is proportional to how richly innervated that region is, not to the body region’s physical size. Areas of the body with greater or more complex sensory or motor connections
are represented as larger in the homunculus such as the hands, lips, and the face.
The primary motor cortex receives signals from the pre-motor cortex to make a movement.
The primary motor cortex then sends the information to make that movement from the cortex down the spinal cord to the skeletal muscle of that body region.
 Motor movement occurs contralaterally, meaning that your left motor cortex controls movement on the right side of your body. Your right motor cortex controls movement on the left side of your body. Every action occurs in this fashion, in response to a descending signal from the brain to the body.
Motor movement occurs contralaterally, meaning that your left motor cortex controls movement on the right side of your body. Your right motor cortex controls movement on the left side of your body. Every action occurs in this fashion, in response to a descending signal from the brain to the body.
Is the Motor Cortex important to Posture?
The motor cortex controls motor function. The Posture System is never actually “static,†we are dynamic beings who are lways in motion. The motor cortex is constantly making small movements (even minute movements) necessary to prevent falling over, and to interact within our environment. Optimal dynamic posture begins in the motor cortex and is regulated by the cerebellum.
Can I check for weakness of the Motor Cortex?
You can check for weakness of motor output by performing muscle tests. If a muscle on the left side is weak,
this is information to do further muscle tests to confirm for weakness of the right motor cortex.
Sensory Cortex:
The somatosensory cortex of the parietal lobe is the center for
sensation. This is where you perceive your world and how you process all of the tactile and
proprioceptive information received from your external environment.
Just as the motor cortex is a map whose arrangement gives preference to the highly innervated parts of the body, so does the sensory homunculus. The sensory homunculus is the primary mechanism of cortical processing for sensoryinformation originating at body surfaces and other tissues.
Is the Sensory Cortex important to Posture?
The sensory cortex is very important for posture because the sensory cortex lights up with activation from novel stimuli such as proprioceptive signals and mechanoreceptor feedback
from complex movements. Lack of movement is the worst thing for your sensory cortex. In fact, with lack of stimulation to an area of the sensory cortex, the sensory map “blurs†together with less representation of that body part in the brain.
For example, when patients present an injured knee and they have worn a brace that limits their range of motion. This limited motor output of the knee results in less tactile and proprioceptive
feedback from the knee, the brain then thinks that the knee is “less important†and blurring of the cortical representation of the hip and ankle will begin to occur over the knee.
Less awareness of our body leads to poor activation and neglect of that area. To keep your patients healthy, keep them moving and activating all joints of the body.
Can I check for weakness of the Sensory Cortex?
You can check for dysfunction of the sensory cortex by performing sensory tests such as light touch,
vibration, temperature, painful stimuli, and joint position. If the patient presents with decreased sensory recognition, the contralateral sensory cortex is weak.
Meaning, that if the left side of the body cannot detect tactile sensation, this is a weakness of the right sensory cortex.
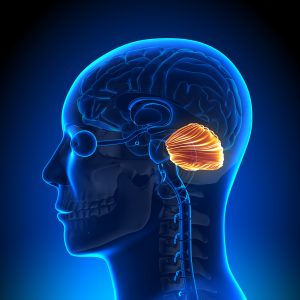
Cerebellum:
The cerebellum works in conjunction with the contralateral motor
cortex to coordinate fine movements. The cerebellum is an “inhibitor,†it reduces any extra or unnecessary motor movements to perform the desired action as accurately as possible.
The cerebellum receives input from sensory systems of the spinal cord and from other parts of the brain, and integrates these inputs to fine-tune motor activity, providing feedback to the motor cortex of how movements can be smoother and more precise. When patients have deficits of the cerebellum
they have excess movement, such as a tremor or a wide stance because they can’t balance with their feet together. Their equilibrium and ability to perform controlled motor movements is compromised.
Is the Cerebellum important to Posture?
The cerebellum coordinates all movement, to more
precisely regulate fine movements. Proper cerebellar output means that the patient can perform their intended movement without recruiting other muscles. They are on target and on point with coordinated functions of the Posture System. Cerebellar deficits on the other hand affect the patient’s posture, they have compromised postural stability and uncoordinated dynamic postures.
Can I check for weakness of the Cerebellum?
You can check for cerebellar weakness by performing a Romberg’s test. Have the patient stand with their feet together, close their eyes, and see if they sway to one side. The patient will sway toward the side of cerebellar dysfunction.
Brainstem:
The brainstem is the center of postural control. The brainstem is made up of the midbrain, the pons, and the medulla and is the house of the nuclei of 10 of 12 of Cranial Nerves.
Each of the cranial nerves provides important sensory and motor functions for the body. Of particular importance to the Posture System are the visual and vestibular nuclei that reside in the brainstem.
The visual system controls your orientation in space, literally how you see the world. Visual fibers descend to the cervical spine controlling head posture. Visual deficits result in forward head posture, lateral head tilt, and head rotation.
The vestibular system controls balance and extension. Flexor dominant posture is weak posture; upright extended posture is healthy and optimal for better function. This system is of utmost importance for upright postural stabilization and balance.
The brainstem also controls involuntary systems of your autonomicnervous system that regulate life-sustaining processes such as breathing, heart rate, sexual function, and digestion. Plus, the brainstem modulates postural tone, and inhibits flexion toward gravity.
Is the Brainstem important to Posture?
This is the primary control center of postural stabilization! The brainstem inhibits flexion, and in conjunction with the vestibular system activates extension. Descending fibers from the cranial nerve nuclei of the eyes control your head posture, and the ability to keep your eyes parallel to the horizon during dynamic movement.
Understanding the brainstem is an important connection for all posture professionals. Your posture depends upon the functional output of the brainstem.
Can I check for weakness of the Brainstem?
Checking posture provides valuable insight into the function of the brainstem. Noted flexion of the Posture System or head posture distortion patterns indicates that there is weakness of the brainstem.
The Cranial Nerves also provide valuable insight of the function of the brainstem. Dysfunction of the cranial nerves means that there is ipsilateral weakness of the brainstem.
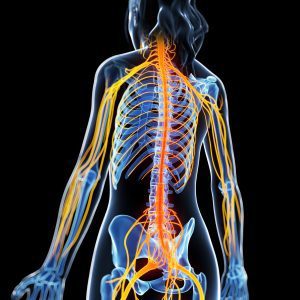
Spinal Pathways:Â
The spinal chord and its pathways are the communication system to and from the brain and the body. The descending motor pathways stimulate movement and postural control. The ascending sensory pathways carry information of sensation to be processed and “understood†in the brain.
The brain and the body are in constant communication to perform efficient movements, to stabilize without falling, and to detect signals from the environment that require a response. Sensorimotor integration happens in your spine, this is the communication highway of the nervous system.
 Are the Spinal Pathways important to Posture?
Are the Spinal Pathways important to Posture?
The pathways are invaluable to your postural design. Pathways from the motor cortex send information to create dynamic movements, and pathways from the brainstem descend to stabilize your postural tone. Ascending pathways from the body to the brain ignite the sensory homunculus for perception, and carry information from the primary sensors of your body for proprioception, vision, hearing, touch, smell, taste, etc.
Can I check for weakness of the Spinal Pathways?
There are many different pathways. When you understand the function of that pathway you can design a test for it. For example, the corticospinal tract descends from the motor cortex to the spine
to create motor output. Dysfunction of this pathway would present as weakness on muscle tests.
The spinothalamic tract is an ascending tract from the spine to the thalamus that recognizes stimuli associated with pain and temperature. To test this tract you would test sensory integration of hot, cold, and painful stimuli.
Sourced through Scoop.it from: www.elpasochiropractorblog.com
Neck pain that is not caused by whiplash or other trauma has a postural component as part of the underlying problem. Sitting atop the body, the health of the neck is subject to the  curvature of the spine below and the position of the head above. For Answers to any questions you may have please call Dr. Jimenez at 915-850-0900
Post Disclaimers
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Poor Posture & Brain Based Postural Correction" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933





 Are the Spinal Pathways important to Posture?
Are the Spinal Pathways important to Posture?




Comments are closed.